Back in February, we were joined by Dr Fiona Jeffries for a Maternity Nurse Masterclass on Perinatal Mental Health as part of our ongoing Continued Professional Development program for Maternity Nurses.
Fiona is a clinical psychologist and owner of ‘Baby Psychology Basics'.
Perinatal Mental Health
Perinatal means ‘around birth'. Mental health refers to our psychological, social, and emotional well-being. Perinatal mental health refers to our psychological, social and emotional well-being from the time of pregnancy through to 12 months postpartum.
It's important to remember that mental health is not a black-and-white concept. There is a real spectrum of mental health and sometimes we are on one side of the spectrum of feeling good, and sometimes we're on the other end of the spectrum where we don't feel so good. This is the same in terms of perinatal mental health. There are lots of words that you might hear used to describe people with specific perinatal mental health conditions, such as perinatal anxiety or postnatal depression or postpartum psychosis.
In this blog post we are focusing on the broader aspect of Perinatal Mental Health:
- Common myths and misconceptions about perinatal mental health.
- How to help parents know when they might want more support.
- How to support parents' bond with their babies when mental health difficulties are present
Mental health difficulty is never the fault of the person who's experiencing it.
Many different factors influence our mental health. Sometimes it can be easy to forget that many different factors influence our mental health.
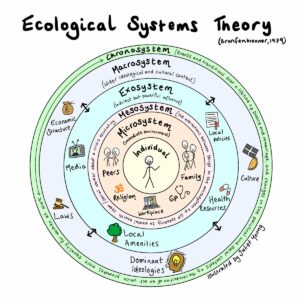
The Ecological Systems Theory, by Psychologist Bronfenbrenner, helps us understand the different influences that impact an individual's mental health. This is helpful when we think about perinatal mental health: we can see an individual in the middle and the various influences which impact their mental health from the closest influencing factors e.g. family, workplace, and social circle. Moving outwardly past factors which have a really powerful influence indirectly on mental health, to the final circle – the Chronosystem, which describes key events that happen in life that have an impact on us. Having a baby is an example of a key component.
There are a variety of influences that can contribute to mental health functions throughout this perinatal period.
Change is constant. Changes can be physical, hormonal, or social. For example, when you become a parent you go through psychological changes in terms of how people feel about themselves and their identity. The transition to motherhood (‘Matrescence') includes all of these changes. All of which can have an impact on our mental health.
A key takeaway message is that perinatal mental health difficulties are really common. A recent study carried out by the Centre of Mental Health conducted ‘Between 10% and 20% of women develop a mental illness during pregnancy or within the first year after having a baby'.

It's really very common to experience difficulties during this period, and one theory addressing why mental health difficulties are so prevalent during the perinatal period is due to the context in which we are having families.
You've probably heard the term “it takes a village to raise a child”.
In today’s society, many people give birth with little social support and may need to return to work soon after giving birth. This is a major contributor to why perinatal mental health difficulties are so prevalent. Traditionally, raising a child was a communal effort, which is where the phrase comes from, and there was more of a focus on recovery after birth, which was possible due to the support received by the new parents.
Common myths and misconceptions
- You can only experience perinatal mental health problems if you have a history of mental health problems. Hopefully, this myth is less prevalent than in previous years, but it's not true. Anyone can experience perinatal mental health difficulties regardless of whether they have a history of mental illness.
- Only a pregnant or birthing person who can experience a perinatal mental health difficulty. As we saw from the statistics above that the prevalence of mental health difficulties in fathers is quite high. And it's only in recent times that this has been getting some attention in the research arena and we must support partners too. There's very little research in terms of same-sex couples. We're at the very beginning of really understanding the impact of these perinatal periods on partners' mental health, but in your roles, it's important to remember to consider the partner if there is one, and how they are, how they may be impacted.Much of the research suggests that if one person is experiencing a mental health difficulty in that partnership, then it becomes more likely that the other partner may also start to struggle with their mental health, which makes sense when considering if you are looking after and witnessing someone you love suffering, that's a difficult thing to go through.
- Parents with postnatal depression don't have moments of joy with their babies or if you are depressed or you have postnatal depression, then you just won't enjoy parenthood. The reality is mental health is not that black and white. If some of the people you are working with are experiencing postnatal depression, they're still able to have moments of joy and cherish those moments. It's also important to acknowledge that sometimes this thought can hinder people from getting help or even recognizing that they need support due to the misconception that if you have postnatal depression, then you are always sad, crying and unable to leave the house. This is commonly not the picture of postnatal depression, often people with postnatal depression do have genuine moments of joy, but often they're also very good at putting a good mask on. They will leave the house, and they might appear as though they are in control, but beneath it all, they are struggling.Not all parents who are experiencing mental health difficulties are going to need professional support. Having a supportive partner or social network, someone who will listen by being there is enough to support them, but at other times it may be helpful for them to get a bit of extra support.
Recognising when parents may need additional support
- If the person you are working with feels they might need some extra support or maybe they feel as though they are struggling, encourage them to trust their instincts, they know themselves better than anybody else. They know what feels comfortable and tolerable and what doesn't. It’s also applicable if they have a supportive partner who notices something isn’t quite right and feels like they need support. Encourage them to trust those instincts and signpost where they can go for some extra support.
- Persistent negative thoughts about their ability as a parent or feeling like a constant failure is another indicator to look out for in your role. We know in these early days and even weeks, it's normal for parents to feel like they have absolutely no idea what they're doing, but often that comes with an acknowledgement that everybody is in the same position in this, nobody knows what they're doing yet. The difference is when somebody may feel that it's a personal failure that they just don't know what they're doing and everybody else does it better than them.
- Another indicator to look out for is if the person you are working for doesn’t want to leave their home, or doesn’t enjoy anything, maybe they feel hopeless or have a constant feeling of anxiety or nervousness.
- Suffering with intrusive thoughts, maybe the person you are working for doesn’t want to spend any time with their baby, or they have thoughts about harm coming to the baby or harming their baby themselves. These intrusive thoughts exist in all areas of life, but people tend not to speak about these thoughts because they're concerned about the reaction of others. It's important to speak about it and to highlight these intrusive thoughts as a normal part of human experience, but equally to recognize that these thoughts are distressing for the person having them. It’s an indicator that this person should seek support and if people are having actual thoughts that they do want to hurt their baby or they want to hurt themselves, then it's important they get support as soon as possible for this.

Is it Baby blues or something more?
‘Baby blues' is a term that refers to often a few days after birth when there are lots of changes to the birthing parents' hormones and often they can feel down and teary. Everybody experiences it differently and some women don't experience baby blues at all.
A common concern is, how do we know if this is normal, if this is just the baby blues or whether we need to do something more about it? Baby blues tend to last only for a few days and then the person feels like they are back to themselves, as normal as they can feel with a new baby.
When each day is affecting them negatively, and they’re feeling similarly over a longer period, if this feeling doesn't dissipate and they're not enjoying daily life or activities, then it could be more than baby blues.
Postpartum Psychosis
One in a thousand women experience postpartum psychosis after birth – a very rare but very serious mental illness. Postpartum psychosis is a severe but treatable form of mental illness that develops after giving birth, very suddenly and often the woman might not have any previous experience with mental illness. Postpartum psychosis normally takes effect during the first few days/weeks after childbirth. It gets worse quickly and should always be treated as a medical emergency. Often it is the people around the person suffering from postpartum psychosis i.e. their partner, or someone from their support network that would be in a position to identify this, the person themselves won't necessarily be in a position to recognize they are not behaving as themselves.
Most women need to be treated with medication and admitted to the hospital. And with the right treatment, women with postpartum psychosis do make a full recovery. Although rare, it’s important to recognise this illness with the woman you're working with so that they can get the support needed straight away. When women do get the right treatment, they often recover very well and fully. For a personal account of Postpartum Psychosis, read this blog by Eve Canavan, one of the founders of Maternal Mental Health Awareness Week and Perinatal Mental Health Partnership.
Signposting for help
Postpartum psychosis symptoms may develop suddenly, the person suffering from postpartum psychosis may experience a mixture of these common symptoms, they might feel; excited, elated, anxious, depressed or confused. They might be; restless, unable to concentrate or sleep. People suffering from postpartum psychosis may also experience, delusions, hallucinations or mania.
- If the woman is still under the midwife's supervision, they will know exactly what to do, speaking to them as a first point of call or their GP. It is treated as a medical emergency; therefore, if their midwife or GP was unavailable, you would contact the emergency services, either 111 or A&E or 999.Every area and location are different. In the UK, most NHS Trusts have a perinatal mental health team which is connected to the mental health services and to the maternity services in that area. The perinatal mental health team consists of a multidisciplinary team of psychologists, mental health nurses, psychiatrists, and nursery nurses who can support bonding and attachment. People often have this idea that mental health services are for people who are having severely difficult mental health issues.Although due to the current strain on the NHS, the reality remains that early intervention is key when it comes to perinatal mental health.
- Clinical psychologists/therapists who specialise in perinatal mental health are private options to consider.
- Many charities support perinatal mental health:
- Pandas
- Best beginnings
- Twins trust
- Mum's Aid
Supporting parents to bond with their baby
Many parents who experience mental health difficulties in this postnatal period question how it might affect their bonding with their newborn. The first thing to highlight is that it doesn't always affect bonding, but it sometimes can make it more difficult. To bond with a baby the parents are needed to provide themselves with enough emotional space and energy to understand how the baby is feeling and what their needs are. Understandably, it’s more difficult to create this space if the parents are feeling extremely low, stressed or worried. You might recognise many of these exercises, you possibly do these to support bonding with families you work with already, the difference would be when you are working with families experiencing mental health difficulties you provide a little extra support.
- Reassure the parent that bonding develops over time. There is this belief that there is this magical moment of falling in love after birth. This happens to some people, but it doesn’t happen to everyone. Relationships take time to develop, encouraging them to continue to go through the motions of speaking with the baby, changing them, dressing them and feeding them and just trust that the emotional connection will come.
- A key thing if you are working with parents during this period when they are struggling with their mental health, is not to separate the parent from their baby. Often, parents are offered some time on their own, perhaps to take a bath, go for a walk on their own or to have a morning off and have a break. If that's what they want and they want some time to themselves to breathe, this can be helpful. But for parents to bond with their babies, they need to spend time with them.Hormones such as oxytocin help the brain sync with the baby. This is done through breastfeeding, holding and cuddling, eye contact, kissing and skin to skin contact. Co-bathing, babywearing and baby massage can also support this process.Parents and their babies are built to be near each other to develop. It helps the body and to mind to feel better. If parents are struggling to bond, then being near the baby as much as possible is one of the ways to help that relationship develop. Although you might have good intentions, separating the parents from their baby can make the bonding process more difficult, which can hurt mental health. Instead, ask yourself how can you support them to spend a bit more time with their baby. That might be helping with ad-hoc washing, cooking and cleaning or supporting them find someone who can support them with those day-to-day chores. Finding ways of supporting them to have time with the baby and look after them. Maybe they hold their baby when they are calm and fed and then you take over when the baby is ready for a nappy change or when they are crying.
- A good social support network is a key factor contributing to bonding between parents and children. Extended family and friends help take care of the practical side of things to give parents time to spend with their babies and bond. Parents feel nurtured and looked after themselves when they have that support network and have the emotional energy to put into their baby. We need to nurture the parents so that they can nurture their baby. Workshop some baby massage techniques with the parents or provide some skin-to-skin ideas.
- Problem-solve the baby’s cues with the parents to help them understand their baby's communication. For example, thinking out loud what the baby wants when they’re crying, maybe they’re hungry or are looking for affection. It can often feel daunting for parents when they don’t know what their baby’s cry means. And it can be a very difficult experience particularly when a parent is struggling to bond. Reassure them that it's OK to not know just yet, and to try a range of things to see what works.
Asking questions is better than making statements.
- Know your boundaries. Know when what a parent is looking for or needs goes beyond what you offer or beyond the scope of your role. Have the confidence to say to signpost accordingly.
- Avoid labelling, your role is not to diagnose. You're there to support the parent and encourage them to choose the words they want to use to describe the experience they're going through. When we are struggling with our mental health, we are very susceptible to feeling like a failure.
- Remember asking questions is better than making statements. For example, you notice a parent you're working with appears low or upset a lot of the time, ask the question, ‘Are you okay?’. Or ask ‘How are you feeling today?”
- Create space for them to let you know whether they are okay or not, everyone experiences emotions in different ways. Everyone’s experience of parenthood is different, be curious and objective rather than drawing on your previous experiences of being a mum if you are a mum or the experiences of other mums that you have worked with.
- Provide them with the correct information to enable them to make the best choice for them.
If you are a member of our Maternity Nurse cohort, you have access to the Masterclass with Dr Fiona in your CPD vault on the platform. If you have an interest in pursuing a career caring for newborn babies, you can download our Maternity Nurse checklist.
Maybe you have a keen interest in psychological difficulties following traumatic childbirth, our Perinatal Mental Health (including Postnatal Depression & Birth Trauma) course looks at the impact of trauma on the brain, body and relationships, as well as assessment tools, the medication used and how to manage risk as a practitioner.